When burnout turns neurological: Autism and FND
Published 27 February 2026
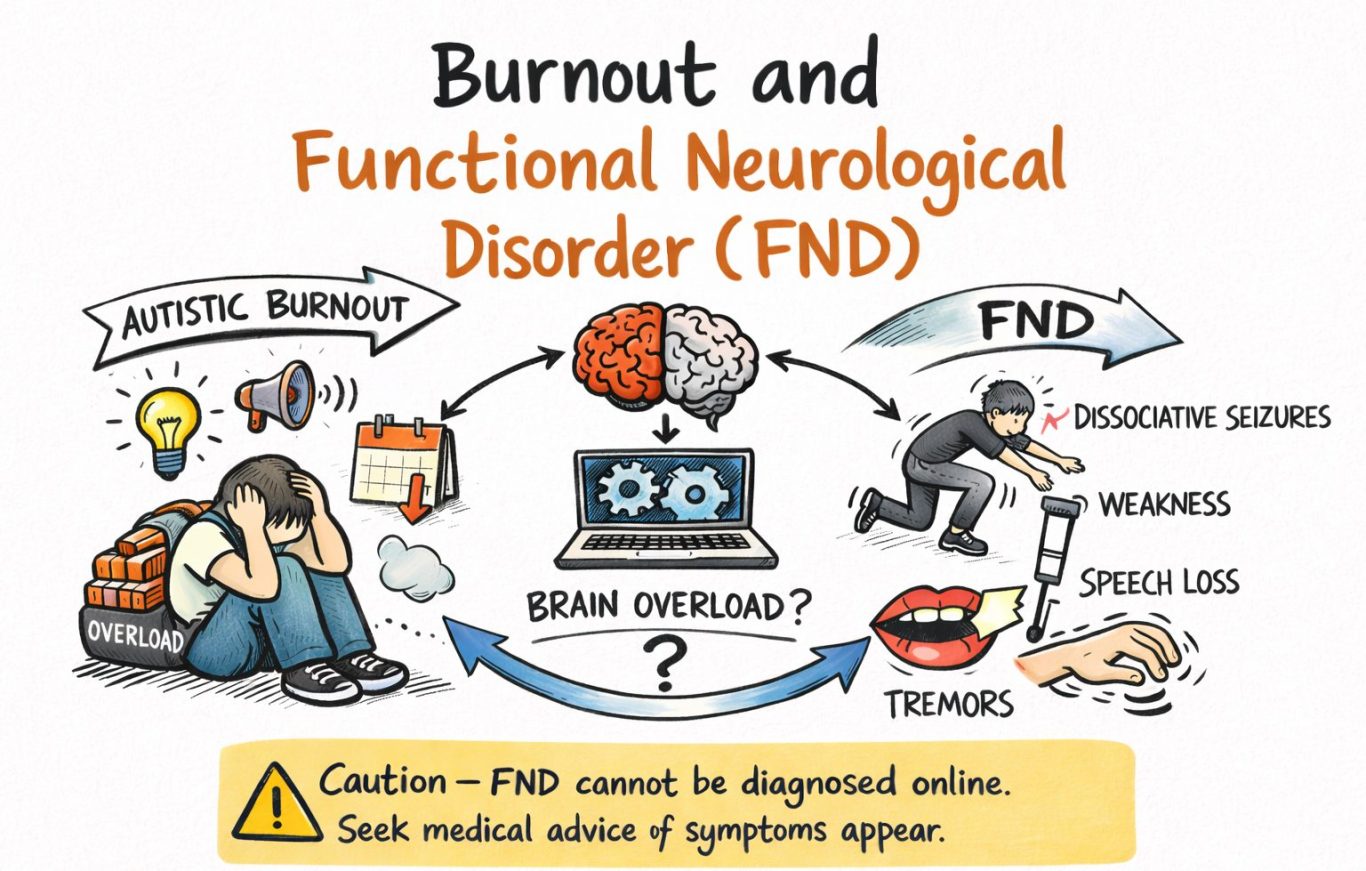
When autistic burnout starts looking neurological: a cautious, human guide to FND-shaped symptoms
A blunt truth first. There is no solid evidence that autistic burnout reliably “turns into” Functional Neurological Disorder (FND). Anyone selling that as a neat pipeline is doing story-telling, not science. What we do have is something messier and still important: (1) a clear research definition of autistic burnout, (2) mainstream clinical descriptions of FND, and (3) a growing body of research suggesting autism and FND co-occur more than you would expect by chance. That combination makes a reasonable working hypothesis: for some autistic people, severe burnout might create a vulnerability state where functional neurological symptoms appear or worsen. Hypothesis, not verdict.
Notice: what autistic burnout actually is
Autistic burnout is not “I’m a bit tired and sick of people”. In the peer-reviewed literature, it is described as a syndrome arising from chronic life stress and a mismatch between expectations and abilities without adequate supports, with pervasive long-term exhaustion, loss of function, and reduced tolerance to stimulus, typically lasting three months or more.
That last bit, reduced tolerance to stimulus, is the quiet killer. When your nervous system is already running hot, “ordinary” environments can become physiologically extreme: noise, light, social demand, time pressure, unpredictability. You can be brave, disciplined, and insightful and still have your capacity collapse. Burnout is not a character flaw. It is an overloaded system doing what overloaded systems do.
What FND is, in plain language
FND is commonly explained as a problem with how the brain sends and receives signals, not a problem caused by structural damage you can see on scans. NHS materials use a “computer” analogy: the hardware is not broken, but the software is not running properly, producing real, involuntary symptoms.
Those symptoms can include weakness, movement problems, sensory changes, speech issues, episodes of altered awareness, and functional (dissociative) seizures.
A key point, often missed in public discussion: FND is not “made up”. It is “functional” in the sense of brain network functioning. Many people improve with the right rehabilitation approach, especially when the diagnosis is explained well and treated without stigma.
Why autism and FND keep turning up in the same room
Research reviews and meta-analyses report that many studies find higher-than-expected rates of autism in FND populations, often summarised around about 10%, while also warning about heterogeneity and possible publication bias.
A 2024 review explores overlaps and hypotheses about why the two might cluster.
A 2025 specialist clinic study used structured assessment and reported “clinically probable ASD” in an adult FND clinic, exploring associations with symptom presentation and factors such as alexithymia and interoception (how you sense internal body states).
None of this proves that burnout causes FND. It does make it sensible, clinically, to take the overlap seriously and to stop acting surprised when people describe “burnout” and “neurological symptoms” in the same sentence.
A cautious model that fits both worlds
Here is a working theory that does not require magical thinking.
- Burnout reduces buffer. Executive function, sensory tolerance, sleep, appetite, coordination, emotional regulation and social coping often degrade together.
- FND is context-sensitive. Symptoms often vary and fluctuate, and the diagnosis is made using positive clinical features, not simply “nothing found”.
- Put together: in a high-load, low-buffer state, brain systems that coordinate movement, speech, attention and perception may become more vulnerable to functional disruption.
This is not “it’s anxiety”. It is not “it’s trauma” either. Psychological factors can be present, absent, central, peripheral, or irrelevant. Contemporary reviews explicitly note that psychological abnormalities are neither necessary nor sufficient for some functional diagnoses, and that attention and expectation can be key ingredients.
What it can look like
What follows are composite, real-life style examples. They are not diagnoses. Their job is to be recognisable and observable.
1) The legs that “work in bed but not in public”
Someone in severe burnout can push their feet against the mattress and move their legs lying down. Then they stand up in a bright, loud supermarket and their knees buckle. They cling to shelves, feel shame burn up their throat, and end up sitting on the floor trying not to cry. Later, at home, they can walk to the kettle. The symptom is real. The pattern is inconsistent across contexts.
Clinicians consider FND when motor symptoms show certain kinds of inconsistency or incongruence with recognised neuroanatomical patterns, and they look for positive signs on examination.
2) Seizure-like episodes that track overload
A person experiences episodes that look like seizures or fainting: shaking, collapse, altered awareness, then heavy exhaustion. They notice clustering after weeks of masking, sleep debt, sensory bombardment, or major transitions. Some later receive the label functional (dissociative) seizures, which epilepsy charities and NHS sources describe as a type of FND.
A necessary safety note: seizure-like events always deserve medical assessment. Autism is associated with higher epilepsy rates than the general population, so “it must be functional” is not a safe assumption.
3) Speech loss: “the words vanish but I’m still here”
In peak burnout, a person becomes intermittently non-speaking, whispers only, stutters severely, or feels their mouth will not cooperate even though they understand everything. They can text, nod, gesture, or write. The loss of speech appears most often in high-demand social settings, appointments, conflict, or sensory overload.
FND descriptions include speech and communication symptoms among possible manifestations.
4) Tremor, jerks, and the body that stops feeling like an ally
A hand tremor appears. It changes with attention. It worsens when observed. It reduces when distracted. The person begins avoiding leaving the house, not because they are lazy, but because the body has become unpredictable.
Functional tremor has well-described positive features such as distractibility and entrainment.
“Positive signs” and Hoover’s sign, without the gotcha vibe
In FND, positive signs are examination findings that help a clinician rule in a functional diagnosis by showing a characteristic pattern: symptoms are real, but they show internal inconsistency or are incongruent with recognised neurological pathways, often changing with attention, distraction, or task demands. NICE CKS explicitly frames diagnosis around positive features, not simply negative tests.
Hoover’s sign is a classic example used in functional leg weakness. If someone appears unable to push one heel down (hip extension) when asked directly, the clinician then asks them to lift the other leg against resistance. In many cases of functional weakness, the “weak” leg automatically pushes down more normally during the effort on the opposite side. This suggests the motor pathways can generate strength even though voluntary, focused movement is disrupted. It can be explained non-judgementally as a problem of movement control rather than muscle power.
A key cultural fix: these signs are not “tricks to catch someone out”. One influential paper argues for showing and explaining signs to patients as part of transparent, therapeutic assessment.
What people report online, and how to treat it responsibly
Social media is not a diagnostic tool. It is, however, a surprisingly good early-warning system for patterns that medicine has not fully mapped yet. On public forums, people repeatedly describe FND diagnoses or FND-type symptoms in the context of autistic overload and burnout: “my FND was triggered by autistic burnout at work”, “I suspect burnout was related to my tics and seizures”, “my symptoms worsen with sensory overload”.
The responsible way to use these narratives is not “look, this proves it”. It is: “there is a recurring lived-experience pattern worth researching and worth keeping on the clinical radar, while still doing proper differential diagnosis”.
A grounded “what to do next” if this sounds familiar
A magazine article is not medical care, so this is deliberately general.
1) Take symptoms seriously, and insist on proper assessment.
If someone in burnout develops new neurological symptoms, the goal is not to pick a label on day one. It is to get careful assessment, because both neurological disease and functional disorders can be serious. FND should not be diagnosed purely from normal tests.
2) Reduce load first, then rebuild function.
If burnout is the fuel, “pushing through” is often the accelerant. Many people improve when they shrink demands, stabilise routines, and work with clinicians who understand both sensory load and rehabilitation. NHS materials emphasise that FND symptoms can reduce or stop with treatment.
3) Treat the nervous system like it learns, because it does.
Functional symptoms can be maintained by fear, hypervigilance, and all-or-nothing cycles. A helpful stance is: real symptom, real nervous system, trainable system. That is neither “it’s all psychological” nor “nothing can be done”.
Closing note
The most honest summary is this: autistic burnout is a prolonged depletion state with reduced tolerance to stimulus; FND is a disorder of brain-body signalling that produces real neurological symptoms; research suggests the two conditions overlap more than expected, and clinical logic suggests burnout may be a vulnerability state for functional symptoms in some people. The humane response is the scientifically sensible one: validate the reality of symptoms, assess properly using positive signs, reduce load, and rehabilitate without shame.
The information in this article is provided for general psychoeducational purposes only. It is not therapy, clinical advice, diagnosis, or a substitute for working with a qualified professional, and it should not be relied on as such. Any examples are illustrative and may not apply to your individual circumstances. If you are considering making changes to your health, wellbeing, relationships, work, or care, seek appropriate professional support tailored to you.
To the fullest extent permitted by law, we accept no responsibility or liability for any loss, harm, or outcome arising from reliance on the contents of this article. If you are in immediate danger or feel unable to keep yourself safe, contact emergency services or your local crisis support line straight away.
© Olena Baeva 2009-2026