When burnout turns neurological: Autism and FND
Published 27 February 2026
A cautious, public-facing guide to FND-shaped symptoms, positive signs, and what to do next.
Caution upfront: Autistic burnout can’t be diagnosed from an article, and Functional Neurological Disorder (FND) can’t be diagnosed online. FND is a rule-in diagnosis made by clinicians using positive signs on examination — not simply because tests are “normal” (see NICE CKS). If you develop new neurological symptoms, seek medical advice.
The moment “burnout” stops sounding like a metaphor
Most people know the word burnout. It often gets used to mean “I’m tired” or “I’m fed up”. Autistic people often mean something else entirely.
Autistic burnout as described in research and lived experience, is not a bad week. It can look like a long, slow systems failure: chronic exhaustion, shrinking tolerance to everyday sensory demands, and a loss of skills you used to have. Cooking becomes impossible. Admin becomes terrifying. Conversation becomes a fog. The nervous system feels like it’s running at above 100% even while you’re doing less and less.
And then, sometimes, something happens that can be genuinely frightening: symptoms appear that look neurological.
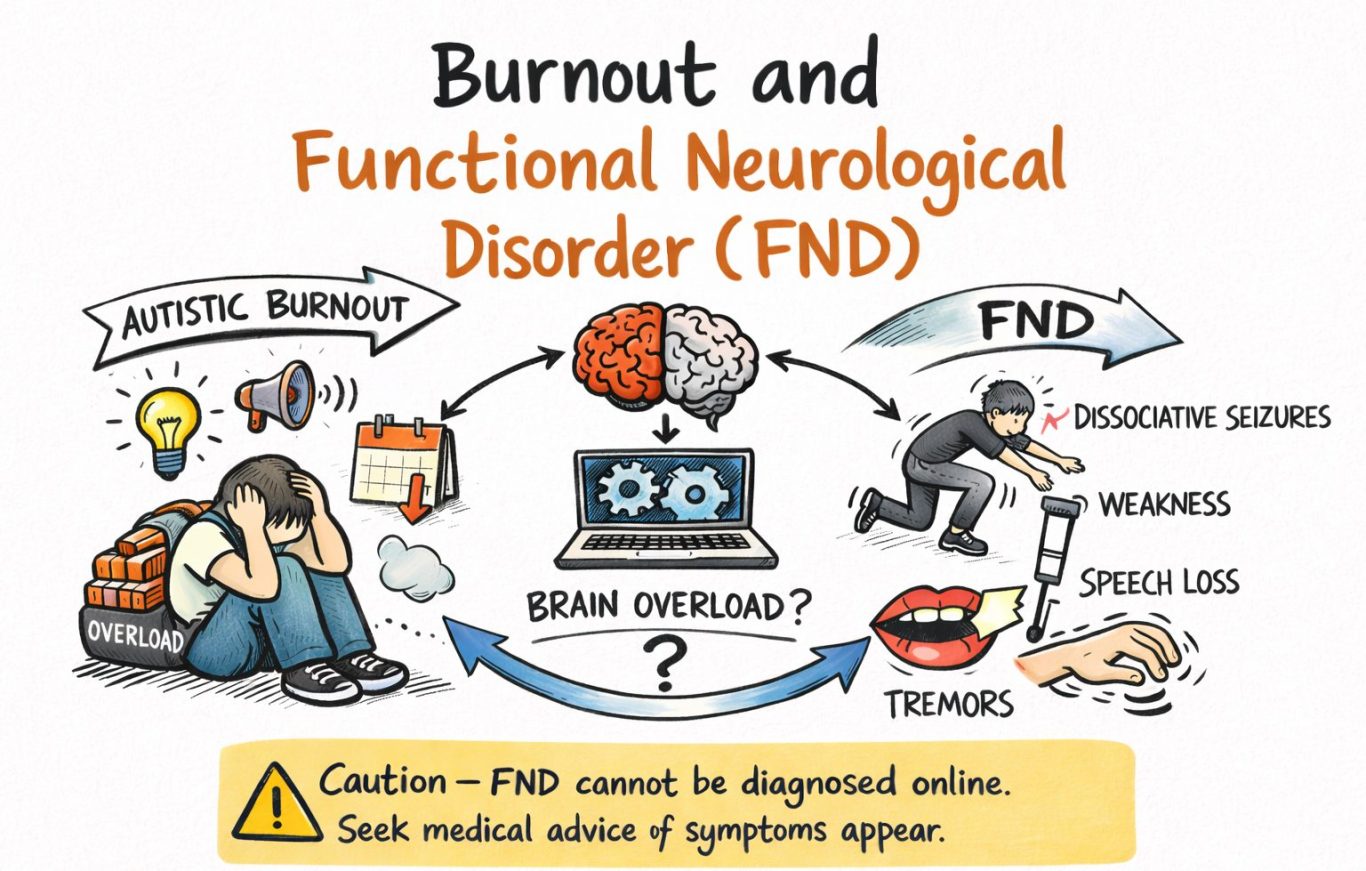
Shaking you can’t control. Episodes that resemble seizures. Weakness or legs that won’t cooperate. Speech that vanishes. Sensory or visual disruption. Dizziness. A body that stops feeling like a reliable ally.
This article offers a careful, non-sensational explanation of a question many people are now asking: Can autistic burnout — at its peak — show up as symptoms that resemble (or overlap with) Functional Neurological Disorder (FND)?
The honest answer is: we don’t yet know in a simple, causal way. But we do have enough evidence to treat the overlap seriously, and enough clinical logic to build a respectful, practical working hypothesis.
Autistic burnout, in plain language
In the peer-reviewed literature, autistic burnout is described as a syndrome arising from chronic life stress and a mismatch between expectations and abilities without adequate supports. It is characterised by long-term exhaustion, loss of function, and reduced tolerance to stimulus, often lasting three months or more.
That “reduced tolerance to stimulus” part matters. When your baseline is already overloaded, ordinary environments can become physiologically extreme: supermarket lights, public transport noise, group chats, workplace politics, constant transitions, having to “perform normal”. Burnout can be the point where the body stops compensating.
What FND is — and what it isn’t
Functional Neurological Disorder (FND) refers to neurological symptoms caused by changes in how the nervous system is functioning, rather than structural damage like a stroke or tumour.
A common clinical analogy is: “software, not hardware.” (See NHS patient information, e.g. NHS Inform.) The hardware (brain structures) may look intact on scans, but the software (how brain networks coordinate signals) is glitching. That glitching is real and can be disabling.
FND can involve symptoms such as weakness or paralysis, tremors, sensory disturbance, vision loss, dizziness, speech changes, and episodes of altered awareness (overview: NHS Inform).
A key point: FND is not “made up”. It’s also not a diagnosis you make because you’ve run out of ideas. Good clinicians look for positive signs — specific patterns on examination that help rule in FND.
Why people are connecting autistic burnout and FND
Here is what the current research can responsibly support:
Evidence is accumulating that autism and FND can co-occur more than expected (review: SAGE paper; meta-analysis: open-access PDF).
The nature of the association remains uncertain — meaning it’s not scientifically clean enough yet to declare a simple pathway (see SAGE paper).
Researchers discuss both endogenous factors (inside-the-body processing differences like interoception) and exogenous influences (outside-the-body realities like adversity, healthcare inequality and stigma) (see SAGE paper).
In other words: the overlap isn’t being framed as “it’s all psychological” and it isn’t being framed as “it’s all biology.” It’s being treated as a whole-system, whole-life question — which is exactly where autistic burnout lives.
A cautious working hypothesis: overload + low buffer
This is the simplest model that stays both humane and scientifically honest:
Burnout reduces buffer. Autistic burnout often includes depleted executive function, sleep disruption, reduced sensory tolerance, reduced capacity for speech and social cognition, and a narrowing window of “I can do this safely.”
FND symptoms are sensitive to context. Many functional symptoms fluctuate and can worsen with fatigue, sensory strain, attention and threat states.
Put together: in a high-load, low-buffer state, some people may become more vulnerable to functional disruptions in movement, speech, sensation, and consciousness.
This does not mean everyone in burnout develops FND. It does not mean symptoms are “just anxiety.” It means that when a system is under sustained strain, the way it coordinates signals can become unstable.
One paper summarises this cautiously: autistic people may be more likely to experience FND, but the reasons are not yet fully understood.
What it can look like in real life
The examples below are composites — built from common patterns described in FND resources and in lived accounts of autistic burnout. They are here to help you recognise a pattern worth assessing, not to diagnose anyone.
1) “My legs work in bed, but not in Tesco.”
Observable: At home, lying down, you can push your feet against the mattress and move your legs. But in a bright, busy supermarket, your knees buckle. Your gait becomes jerky or frozen. You feel like you’re walking through glue. You end up sitting on the floor — not dramatically, but because your body refuses.
Why this pattern raises FND on the radar: Clinicians look for inconsistencies and incongruences with known neurological pathways — not as a “gotcha”, but as evidence of a functional movement control problem.
How burnout could be relevant (speculative): supermarkets are sensory warfare. Burnout shrinks tolerance. Add time pressure and social fear, and the motor system can destabilise.
2) “I have episodes that look like seizures when I’m overloaded.”
Observable: You collapse, shake, lose awareness or become unresponsive, then wake exhausted. They cluster during sleep debt, sensory overwhelm, conflict, major transitions, or after weeks of masking.
Some people later receive a diagnosis of functional (dissociative) seizures — a form of FND (patient explainer: Epilepsy Action on dissociative seizures/NEAD).
Safety note: seizure-like episodes must be medically assessed. Autistic people can also have epilepsy. Never assume.
3) “My words vanish, but I’m still here.”
Observable: During appointments, conflict, or sensory overload, you can’t speak — or can only whisper. You can still understand everything. You can text, nod, gesture, write. But speech production collapses.
How burnout could be relevant (speculative): speech is expensive. It needs breath control, motor planning, timing, and social prediction. Burnout leaves fewer resources for that orchestration.
4) “My hand shakes, and it changes when I stop focusing on it.”
Observable: a tremor appears. It worsens when you’re watched. It changes when you’re distracted. It might synchronise with a rhythm in the other hand.
This can be frightening, especially if you’ve been taught that neurological symptoms always mean degeneration.
Why clinicians think ‘functional tremor’: functional tremor has positive features such as distractibility and entrainment.
Distractibility (lay terms): the tremor may reduce or change when your attention is pulled elsewhere — not because you’re faking, but because the motor system behaves differently when it isn’t spotlighting the symptom.
Entrainment (lay terms): the tremor may sync to an external rhythm — for example, matching a tapping beat in the other hand — whereas many structural tremors keep a more fixed rhythm.
What “positive signs” and Hoover’s sign mean
In FND, positive signs are examination findings that help clinicians rule in a functional diagnosis by showing a characteristic pattern: symptoms are real, but they show internal inconsistency or are incongruent with known neurological pathways. The symptom may change with attention, distraction, or task context.
One classic example in functional leg weakness is Hoover’s sign.
Hoover’s sign (lay explanation): (friendly explainer: neurosymptoms.org) If someone seems unable to push one heel down when asked directly, a clinician then asks them to lift the other leg against resistance. In many cases of functional weakness, the “weak” leg automatically pushes down more normally during the effort on the opposite side. That shows the motor pathways can generate strength, even though voluntary, focused movement is disrupted.
These signs are not “tricks” to catch people out. They’re ways to identify a treatable movement control problem and explain it without blame.
Social media stories: signal, not diagnosis
Online narratives can’t confirm FND. Diagnosis needs clinical assessment and positive signs. But social media can still reveal patterns worth researching.
Across many public accounts, people describe:
severe autistic burnout (masking, chronic stress, demands without supports)
neurological-looking symptoms (dissociative seizures, weakness, gait changes, speech loss, tremor)
trigger sensitivity (worsening with sensory overload, stress, fatigue, being watched)
The responsible use of these stories is not “this proves it.” It’s: this overlap keeps appearing, and clinicians and researchers should take it seriously (see also the 2025 specialist clinic paper on ASD traits in an FND clinic: Scientific Reports).
What to do if this sounds familiar
1) Take symptoms seriously without rushing to a label
If you develop new neurological symptoms, the goal is not to win a diagnosis online. It is to get careful assessment. FND is a valid possibility, but so are many other conditions.
2) Reduce load first, then rebuild function
If burnout is the fuel, “pushing through” is often the accelerant.
A stabilising sequence many people find safer is:
Shrink demands and reduce sensory exposure where possible.
Protect sleep and basic physiology.
Pace to avoid boom-and-bust cycles.
Rebuild capacity gradually with support.
If FND is diagnosed, rehabilitation approaches (often physiotherapy/OT and sometimes psychological therapy) can help retrain movement, attention, and threat-state patterns.
3) Use language that lowers threat
A nervous system learns from experience. Shame and panic increase threat load.
Try:
“This symptom is real.”
“My nervous system is overloaded.”
“Smaller steps are still steps.”
“I’m training safety, not forcing performance.”
A final, honest summary
Autistic burnout is a prolonged depletion state with reduced tolerance to stimulus and real loss of function. FND is a disorder of brain-body signalling that produces real neurological symptoms, diagnosed using positive signs.
Research suggests autism and FND overlap more than expected — but the nature of the association remains uncertain. The most defensible public-facing conclusion is this:
In some people, severe burnout may act as a vulnerability state for functional neurological symptoms — not because symptoms are imagined, but because the nervous system is running beyond capacity.
The humane response is the scientifically sensible response: validate symptoms, assess properly, reduce load, and rehabilitate without shame.
The information in this article is provided for general psychoeducational purposes only. It is not therapy, clinical advice, diagnosis, or a substitute for working with a qualified professional, and it should not be relied on as such. Any examples are illustrative and may not apply to your individual circumstances. If you are considering making changes to your health, wellbeing, relationships, work, or care, seek appropriate professional support tailored to you.
To the fullest extent permitted by law, we accept no responsibility or liability for any loss, harm, or outcome arising from reliance on the contents of this article. If you are in immediate danger or feel unable to keep yourself safe, contact emergency services or your local crisis support line straight away.
© Olena Baeva 2009-2026